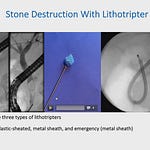
The Promise of Seeing What Only the Microscope Can See
Imagine you’re mid-procedure, staring at a suspicious colorectal polyp. You know a biopsy means days of waiting—and a second procedure if the result demands resection. What if your endoscope could function as a microscope, delivering a histologic-grade diagnosis in real time? That is the central question driving decades of innovation in endoscopic imaging.
In this lecture, Dr. Klaus Mönkemüller traces the evolution of endoscopic visualization—from early fiber-optic magnification and dye-based chromoendoscopy to modern mega-magnification technologies like confocal laser endomicroscopy and endocytoscopy—and asks whether we have finally arrived at true “virtual histology.”
The Three Objectives of Endoscopy
Before exploring advanced imaging, Dr. Mönkemüller grounds the discussion in the foundational goals of the discipline. The objectives of endoscopy are threefold:
“Reach a visual diagnosis.”
“Assist in obtaining a histopathologic diagnosis”—generally by obtaining biopsies and sending them for analysis.
“Provide therapy (and palliation).”
The quest for improved endoscopic visualization has been ongoing since the origins of camera and fiber-optic endoscopy. Dr. Mönkemüller references elegant studies from Japan, dating back more than thirty years, that already demonstrated magnification endoscopy combined with dye application to characterize the mucosa.
Decoding the Mucosa: Patterns and Capillaries
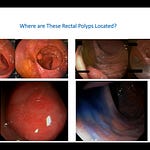
To achieve a visual diagnosis, endoscopists must focus on two primary mucosal features: mucosal surface patterns and capillary patterns. These are the key elements for recognizing abnormal pathology.
Pit patterns become distorted in cases of neoplasia. And since the classic article by Volkmann in the New England Journal of Medicine in 1974, angiogenesis has been recognized as a hallmark of neoplasia—meaning neovascularization is a critical finding.
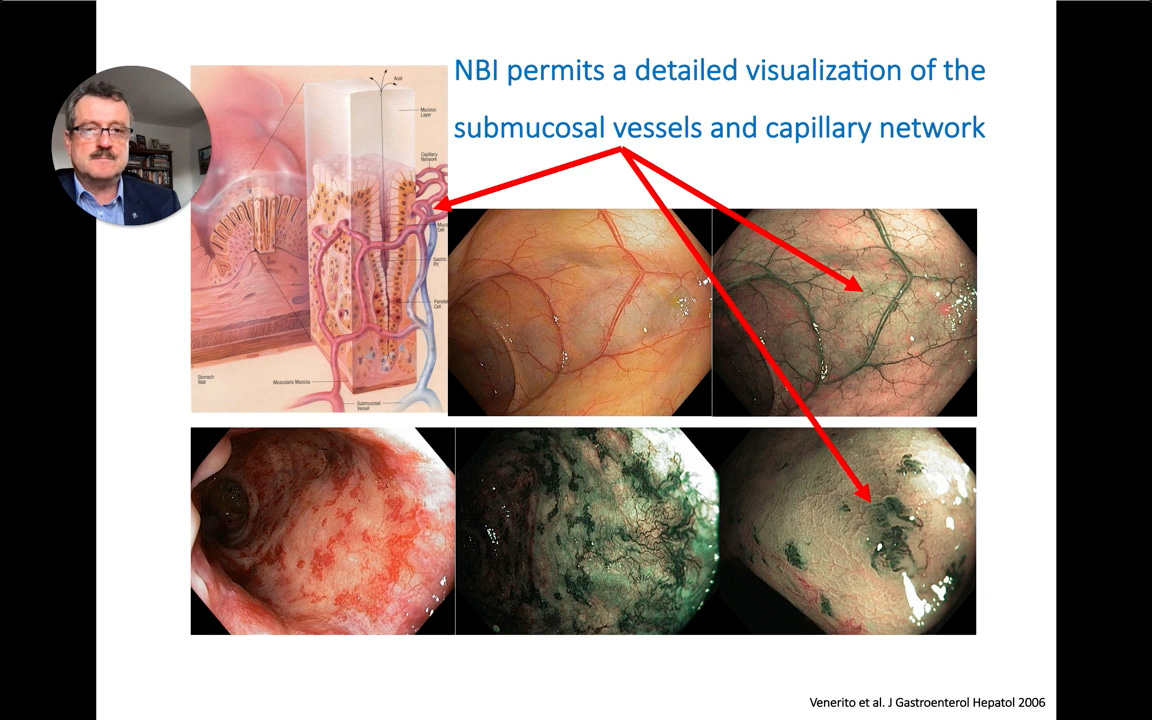
Narrow-band imaging (NBI) permits detailed visualization of submucosal vessels and the capillary architecture—the foundation of pattern-based diagnosis.
First Take-Home Message:
“Visualization can be improved by changing or adjusting essential photographic principles such as: light, focus, shadows, contrast and size (magnification).”
Endoscopic Microanatomy: Where Patterns Meet Histology
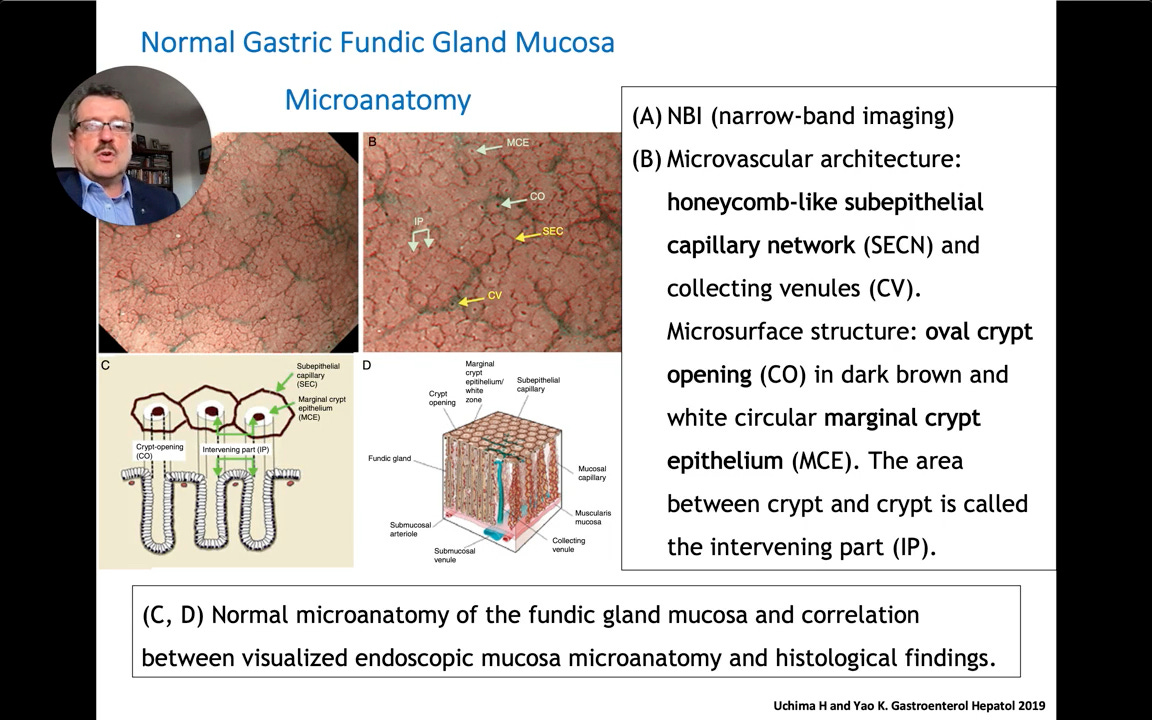
By examining the subepithelial capillary network, endoscopists can observe specific microanatomic patterns. Dr. Mönkemüller highlights a review by Uchima and Yao demonstrating that the microvascular architecture of the stomach resembles honeycombs, with oval crypt openings and marginal crypt epithelium.
These endoscopic patterns correlate perfectly with true histological findings. In Dr. Mönkemüller’s own PhD research on non-erosive reflux disease, red streaks visualized via magnification endoscopy directly corresponded to histological elongation of the papillae—establishing clear endoscopic-histologic correlates.
Practical Application: The JNET Classification
Pattern recognition directly drives therapeutic decisions. If an endoscopist identifies a JNET Type 3 pattern on a colorectal polyp, it indicates invasion and neoplasia—and standard endoscopic surgery will not be helpful for that patient.
Second Take-Home Message:
“There are clear histopathologic correlates of endoscopic imaging (the concept of ‘endoscopic microanatomy’), which assist in diagnosis and therapeutic decision-making.”
To see advanced comparisons between endomicroscopy and endocytoscopy, the role of AI, and a downloadable quick-reference guide based on this video, consider becoming a paid subscriber.